Whiplash is one of the most under-treated injuries we see at CJW. Most people walk away from a low-speed rear-end thinking they're fine because nothing hurts in the moment — and 24, 48, or 72 hours later, they wake up unable to turn their head. By then they've slept on it, gone back to work on it, picked their kids up on it, and the soft tissue has had three days to lock down. The window where this is easy to fix is the first three days. Here's how to use them.
What whiplash actually is
Whiplash is a soft-tissue injury caused by rapid acceleration-deceleration of the head and neck. In a rear-end collision, your torso gets pushed forward by the seat in roughly 50 milliseconds. Your head — which weighs about as much as a bowling ball — doesn't get the same push, so for a few hundredths of a second your neck has to violently catch up. The cervical spine snaps backward (extension), then rebounds forward (flexion), tearing or straining the small ligaments that hold each vertebra to the next, the deep stabilizing muscles of the neck, the joint capsules, and sometimes the discs themselves.
Speed of impact matters less than people think. Studies have documented clinically significant whiplash from rear-end collisions at as low as 5–10 mph. The reason: your seat is the spring, your seatbelt holds your hips, and your head is the unrestrained mass at the end of the lever. Property damage on the bumper is a poor predictor of damage to your neck.
Why pain is delayed — and why that's the trap
Adrenaline and cortisol surge during a collision and stay elevated for several hours afterward. They mask soft-tissue pain almost completely. As those stress hormones drop overnight, inflammation moves in, and the strained ligaments and muscles report what actually happened. That's why most whiplash patients feel okay at the scene, mildly stiff that evening, and considerably worse by the next morning. The pain isn't 'getting worse' — it's finally being felt.
Hour-by-hour: what to do (and what not to)
0–2 hours: at the scene and just after
- Get checked at the scene if there's any loss of consciousness, confusion, severe headache, weakness, numbness, vision changes, or significant pain — call 911 and accept the EMS evaluation.
- Photograph the inside and outside of both vehicles before they're moved. The angle of the seats and headrest position matters later.
- Decline the urge to say 'I'm fine' to the officer or the other driver. Say 'I'm not sure yet — I'll get evaluated.' That phrase doesn't admit injury, but it doesn't waive your right to claim one if symptoms emerge.
- Do not refuse transport if EMS recommends it. The cost of a ride that turns out to be unnecessary is small. The cost of skipping a transport with an actual concussion is not.
2–12 hours: the first afternoon and evening
- Apply ice to the back of your neck for 15 minutes, every hour or two. The goal is to slow the inflammatory cascade before it sets in. Skip heat for at least the first 24 hours — heat at this stage adds blood flow to tissue that's already swelling.
- Stay hydrated and eat a real meal. Soft tissue healing needs protein and water; this is not a day to skip dinner.
- Move gently. Walk around the house. Make slow, small head turns within a comfortable range — pain is the limit, not the goal. Total stillness is what makes this stiffen up overnight.
- If you take an NSAID like ibuprofen, take it with food and a full glass of water. Acetaminophen is fine but won't reduce inflammation.
- Avoid alcohol. It thins blood, increases swelling, and masks symptoms you need to be watching for.
- Do not get a deep-tissue massage today. The tissue is bruised internally; aggressive pressure will make it worse before it gets better.
12–24 hours: the first night and morning after
- Sleep on your back if you can, with a single thin pillow under your head and a small rolled towel under your neck for support. Side sleepers should use a pillow that keeps the neck level with the spine.
- Skip stomach sleeping entirely tonight. It forces your neck into 90° of rotation for hours.
- In the morning, expect more pain and stiffness than you went to bed with. This is normal and is not, by itself, a sign things are getting worse — it's the inflammation peaking.
- Do five gentle range-of-motion movements in bed before you stand: chin tucks, slow head turns each direction, slow ear-to-shoulder each side, and small shoulder rolls. Twenty seconds total. This is not a workout — it's a wake-up.
- Switch from ice to alternating ice/heat after the 24-hour mark if swelling has settled. Ten minutes ice, ten minutes off, ten minutes warm.
24–48 hours: the second day
- Get evaluated. Even if you feel manageable, this is the right window for a chiropractic or musculoskeletal physician's exam. We can identify what's actually injured (ligament vs muscle vs joint vs disc), document baseline range of motion for any future insurance claim, and start the right treatment before tissue locks down.
- If you can, take it easy at work. Email is fine. Anything that requires sustained neck flexion (looking down at a phone, reading printouts on a desk) for more than 20 minutes will set you back.
- Continue gentle movement every couple of hours. Walking is the single best thing you can do for whiplash on day two.
- Don't drive long distances yet. Reaction-time studies show measurable degradation in shoulder-checking ability for the first 5–7 days after even mild whiplash.
48–72 hours: the third day
- By now, pain should have plateaued or begun to slowly improve. If pain is still climbing on day three, that's a signal to escalate care, not to wait it out.
- Begin gentle isometric strengthening only if cleared by your provider — palms-on-forehead resistance, palms-on-temples resistance, ten seconds each, three reps. No movement, just resistance. This wakes the deep cervical stabilizers without aggravating the strain.
- Don't return to the gym, run, lift weights, or play with kids on your shoulders yet. Three days is when you stop being acutely injured. It's not when you're healed.
Red flags — stop reading and go to the ER
Most whiplash is soft-tissue and resolves with conservative care. A small percentage masks something more serious. If any of the following are true, do not drive yourself; call 911 or have someone take you to the nearest emergency department immediately.
- Loss of consciousness at any point during or after the collision
- Severe or worsening headache, especially one that came on suddenly
- Vomiting more than once, confusion, slurred speech, or trouble understanding what people are saying
- Weakness, numbness, or tingling in an arm or leg — particularly if it's getting worse rather than better
- Loss of bladder or bowel control, or saddle-area numbness
- Vision changes, double vision, or unequal pupil size
- Inability to turn your head at all, or sharp electric pain when you try
- Bruising behind the ears or around the eyes that wasn't there immediately after impact
“Nine out of ten patients I see in week one tell me they almost didn't come because they didn't think it was a big deal. Of those nine, every single one is glad they came. The other one is the patient I send to the ER.”
— Dr. Williams
Where chiropractic fits in the first 72 hours
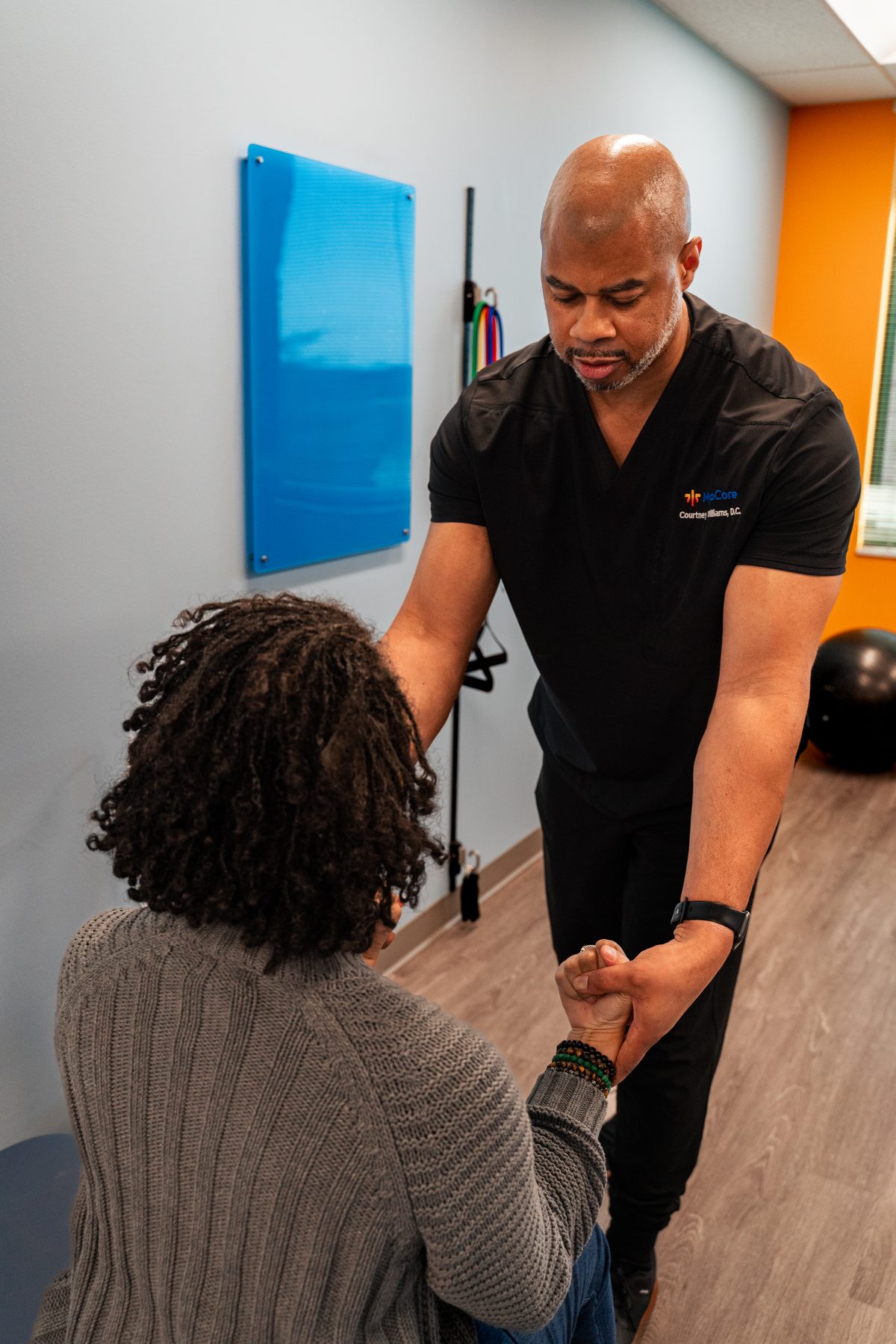
A common misconception is that chiropractic = high-velocity neck manipulation, and that anything cracking on a recently-injured neck must be a bad idea. Both halves of that are wrong. We do not high-velocity manipulate an acutely whiplashed cervical spine. We do, in the first 72 hours, do something much more useful: a proper exam, gentle joint mobilizations to keep segments from locking down, light soft-tissue work to reduce muscle guarding, and instrument-assisted or drop-table adjustments where they're indicated. None of that involves twisting your neck.
More importantly, an early visit lets us document objective baseline measurements — cervical range of motion, neurological screen, pain map — that almost no other provider takes the time to capture. If the case becomes an insurance or legal matter later, that documentation is the difference between a settled claim and a denied one. We coordinate notes back to your PCP and to your attorney's office if you have one.
What treatment looks like over the first six weeks
- Week 1–2: 2–3 visits per week. Pain control, soft-tissue work, gentle mobilizations, posture and sleep coaching.
- Week 3–4: 1–2 visits per week. Range-of-motion work, deep cervical stabilizer activation, return to light activity.
- Week 5–6: 1 visit per week. Strengthening progression, return to gym/sport, re-measure baseline metrics.
- Most uncomplicated whiplash cases close out around week 6. The cases that don't are usually the ones that waited two or three weeks before getting started.
On insurance and cost
Texas is a fault state. If the other driver was at fault, their auto liability policy is generally responsible for your medical bills (subject to their limits). Your own MedPay or PIP coverage, if you carry it, can pay your bills regardless of fault. CJW works with most major auto carriers and with personal-injury attorneys directly — we can verify your coverage on your first call so you know what's covered before you commit to anything.
Common questions
The takeaway
If you've been rear-ended in the last three days and you're reading this, here's the honest summary: your neck is probably injured even if it doesn't feel like it yet, the easy treatment window is short, and the documentation you create in week one is the documentation an adjuster looks at in month six. Get ice on it tonight, sleep on your back, and book an evaluation tomorrow. We'll handle the rest.
Ready when you are
Book a 108-dollar evaluation.